December 2023
Athlete’s Foot Causes and Risk Factors
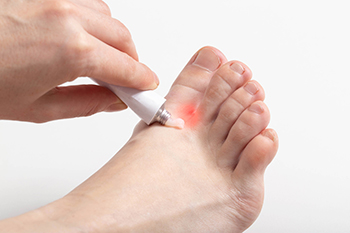
Athlete's foot, a common fungal infection of the skin, is primarily triggered by dermatophytes, which are fungi that infiltrate the skin through small cracks or wounds. These unwelcome invaders thrive in warm and moist environments, making your feet an ideal breeding ground for athlete’s foot. The constant warmth and moisture created by wearing shoes and socks for extended periods provide the perfect conditions for these fungi to flourish. The fungi feed on keratin, a protein abundant in the top layer of your skin. Transmission occurs through direct skin contact or exposure to infectious skin flakes, such as those found in communal showers. Several risk factors elevate the likelihood of developing athlete's foot. A genetic predisposition, allergies, eczema, and excessively sweaty feet are common factors. A weakened immune system, circulation problems, and engagement in certain sports such as running and swimming are also contributors. Individuals constantly wearing sturdy footwear, such as safety or rubber boots, face an elevated risk. For help in managing stubborn or continual cases of athletes’ foot, it is suggested that you schedule an appointment with a podiatrist.
Athlete’s Foot
Athlete’s foot is often an uncomfortable condition to experience. Thankfully, podiatrists specialize in treating athlete’s foot and offer the best treatment options. If you have any questions about athlete’s foot, consult with Gregory T. Loo, DPM from Elite Podiatry. Our doctor will assess your condition and provide you with quality treatment.
What Is Athlete’s Foot?
Tinea pedis, more commonly known as athlete’s foot, is a non-serious and common fungal infection of the foot. Athlete’s foot is contagious and can be contracted by touching someone who has it or infected surfaces. The most common places contaminated by it are public showers, locker rooms, and swimming pools. Once contracted, it grows on feet that are left inside moist, dark, and warm shoes and socks.
Prevention
The most effective ways to prevent athlete’s foot include:
- Thoroughly washing and drying feet
- Avoid going barefoot in locker rooms and public showers
- Using shower shoes in public showers
- Wearing socks that allow the feet to breathe
- Changing socks and shoes frequently if you sweat a lot
Symptoms
Athlete’s foot initially occurs as a rash between the toes. However, if left undiagnosed, it can spread to the sides and bottom of the feet, toenails, and if touched by hand, the hands themselves. Symptoms include:
- Redness
- Burning
- Itching
- Scaly and peeling skin
Diagnosis and Treatment
Diagnosis is quick and easy. Skin samples will be taken and either viewed under a microscope or sent to a lab for testing. Sometimes, a podiatrist can diagnose it based on simply looking at it. Once confirmed, treatment options include oral and topical antifungal medications.
If you have any questions, please feel free to contact one of our offices located in Ahwatukee, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What to Do About Cracked Heels
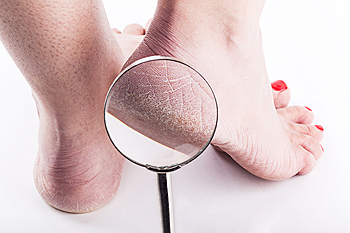
Cracked heels, a common foot condition, often result from dry and thickened skin surrounding the heel edge. While they may primarily affect appearance, they can lead to discomfort or pain and even severe issues, if left untreated. Cracked heels are often caused by dry skin, obesity, wearing poorly fitting shoes, or standing for extended periods of time. Certain conditions and risk factors may increase susceptibility. Women are more susceptible to this condition. Managing cracked heels involves actions that can include moisturizing, wearing 100 percent cotton socks, and gently rubbing thickened skin with a pumice stone. Medical treatments may be necessary for severe cases, including dead skin removal and antibiotic treatment for infections. If you have cracked heels and the condition is associated with a medical condition, or if they are persistent and severe, it is suggested that you schedule an appointment with a podiatrist for more professional guidance.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact Gregory T. Loo, DPM from Elite Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact one of our offices located in Ahwatukee, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Causes of Foot Corns
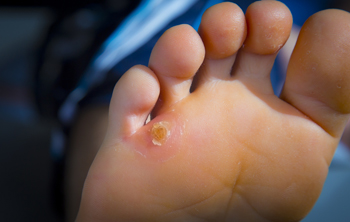
A foot corn, medically known as a heloma, is a common foot condition characterized by a localized thickening of the skin that usually occurs on the feet or toes. These corns are typically small, circular, or conical in shape, and may have a central core of hard, dense material. The two primary types of foot corns are hard corns and soft corns. Hard corns often form on the tops or sides of toes and the balls of the feet, appearing as yellow or gray, dense patches of skin. Soft corns tend to develop between the toes in moist, sweaty areas, having a softer, more rubbery texture. The main cause of foot corns is persistent friction and pressure on the skin, often due to wearing ill-fitting shoes, high heels, toe deformities, walking abnormalities, or excessive moisture exposure. If corns develop on your feet and become painful, it is suggested that you schedule an appointment with a podiatrist who can recommend appropriate treatments and measures for relief. These may include wearing protective pads, cushioning, orthotics, or, in some cases, professional corn removal.
If you have any concerns regarding your feet and ankles, contact Gregory T. Loo, DPM of Elite Podiatry. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
- Well-fitting socks
- Comfortable shoes that are not tight around your foot
- Shoes that offer support
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact one of our offices located in Ahwatukee, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Laser Treatment for Toenail Fungus
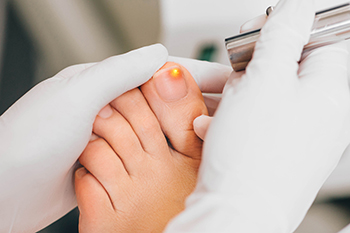
Laser treatment for toenail fungus has emerged as an innovative approach to tackling this persistent and often stubborn condition. This non-invasive procedure involves using focused laser beams to target and eradicate the fungal infections that reside beneath the toenail. The laser energy penetrates the nail plate, reaching the affected area without causing harm to the surrounding healthy tissue. The heat generated by the laser effectively kills the fungus, offering a promising alternative to traditional treatments such as oral medications or topical solutions. Multiple sessions may be required for optimal results. However many individuals find laser treatment appealing due to its minimal side effects and the absence of the potential liver complications associated with oral medications. Understanding this procedure provides individuals with valuable insights into a contemporary and effective solution for addressing toenail fungus and restoring clear, healthy nails. If you have developed toenail fungus and would like detailed information about this type of treatment, it is suggested that you schedule an appointment with a podiatrist.
Laser treatment can be an effective way to get rid of toenail fungus. If you have any questions about laser treatment, consult with Gregory T. Loo, DPM from Elite Podiatry. Our doctor will assess your condition and provide you with quality treatment for fungal nails.
What Are Toenail Fungal Infections?
Onychomycosis, or fungal infection of the nail, is a relatively common and non-serious condition. Around 10 percent of U.S. citizens are afflicted with fungal nails. Common forms of fungus that infect the nail include dermatophytes, yeasts, and molds.
Symptoms of Toenail Fungal Infections Include:
- Nail thickening
- Brittleness of the nail
- Discoloration of the nail
Diagnosis for Fungal Nails
Fungal infections are diagnosed by fungal culture and microscopy. This will rule out any other conditions such as nail trauma, psoriasis, lichen planus, and onychogryphosis.
What Is Laser Treatment?
Laser treatment is a non-invasive, safe, quick, and painless procedure that uses the heat from a laser to kill fungus in the nail. Each infected nail is targeted with a laser for several minutes. The treatment is usually utilized several different times over a select period. During this time, a podiatrist will keep an eye on the infection.
If you have any questions, please feel free to contact one of our offices located in Ahwatukee, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot care needs.