Ways to Care For the Feet as They Age
 Over time, the feet begin to develop more problems due to everyday wear and tear. There is more stress placed on the joints in the feet, and the skin gets thinner and loses its elasticity. Because of the variety of debilitating foot issues that can occur with aging, it is important that elderly patients take care of their feet. Common issues that indicate aging feet include aches and pains, bunions, circulatory issues, and a curling up of the toes. Exercise, proper toenail trimming, moisturizing the feet, and wearing shoes that are supportive and that fit correctly are a few ways to minimize the effects of aging on the feet. Doing yearly checks with a podiatrist is another effective way to help care for the feet. A podiatrist can help detect a variety of issues that include diabetes and poor circulation, and they can help treat everyday foot problems like bunions and ingrown toenails.
Over time, the feet begin to develop more problems due to everyday wear and tear. There is more stress placed on the joints in the feet, and the skin gets thinner and loses its elasticity. Because of the variety of debilitating foot issues that can occur with aging, it is important that elderly patients take care of their feet. Common issues that indicate aging feet include aches and pains, bunions, circulatory issues, and a curling up of the toes. Exercise, proper toenail trimming, moisturizing the feet, and wearing shoes that are supportive and that fit correctly are a few ways to minimize the effects of aging on the feet. Doing yearly checks with a podiatrist is another effective way to help care for the feet. A podiatrist can help detect a variety of issues that include diabetes and poor circulation, and they can help treat everyday foot problems like bunions and ingrown toenails.
Proper foot care is something many older adults forget to consider. If you have any concerns about your feet and ankles, contact Gregory T. Loo, DPM from Elite Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
The Elderly and Their Feet
As we age we start to notice many changes in our body, but the elder population may not notice them right away. Medical conditions may prevent the elderly to take notice of their foot health right away. Poor vision is a lead contributor to not taking action for the elderly.
Common Conditions
- Neuropathy – can reduce feeling in the feet and can hide many life-threatening medical conditions.
- Reduced flexibility – prevents the ability of proper toenail trimming, and foot cleaning. If left untreated, it may lead to further medical issues.
- Foot sores – amongst the older population can be serious before they are discovered. Some of the problematic conditions they may face are:
- Gouging toenails affecting nearby toe
- Shoes that don’t fit properly
- Pressure sores
- Loss of circulation in legs & feet
- Edema & swelling of feet and ankles
Susceptible Infections
Diabetes and poor circulation can cause general loss of sensitivity over the years, turning a simple cut into a serious issue.
If you have any questions please feel free to contact one of our offices located in Ahwatukee, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Elderly and their Feet
While proper foot care is important for everybody, senior citizens have the tendency to be more susceptible to certain foot conditions. The elderly should therefore be well informed about any problems that may arise and about what they can do to properly avoid or treat them.
Some of the most common foot problems seniors are susceptible to include foot ulcers, ingrown toenails, fallen arches, and fungal nails. A foot ulcer is an open sore on the foot and can be a result of diabetes and decreased sensation in the feet. An ingrown toenail is defined as when the nail grows into the side of the toe. Fallen arches are indicated by the instep of the foot collapsing. A fungal nails is a condition that results in deformed and discolored toenails.
In order to avoid these conditions it is recommended that the feet be inspected by the patient on a regular basis. If these inspections are carried out routinely, there is a good likelihood that problems can be identified before they become severe, or can even be avoided altogether. If any abnormality is discovered, it is important that the individual consult a podiatrist for diagnosis and information on treatment options.
Proper foot hygiene is also important. Making sure that you always have clean, dry socks on can be a major deterrent to many different problems including bacterial infections, foot odor, and certain types of fungus. Wet feet are a major cause of many of these problems. If your socks get wet, it is important to change them. Walking around in wet socks may not only lead to various infections, but can irritate the skin and result in a number of various complications. Clean, dry feet are less likely to be affected by fungal and other infections.
As people age, the fat present on your feet begins to deteriorate. The protective nature of this fat keeps the feet healthy by providing a barrier between your bones and the ground. This also aids in giving the skin on the feet a certain amount of elasticity. This is one factor that causes elderly people to develop some serious foot issues. Foot moisturizers can be helpful to avoid certain problems associated with this. However, water-based moisturizers do not work as well for elderly people as they do for the young. Instead, it is more effective to use an emollient instead. An emollient is effective because it binds the water in the foot, keeping it from becoming absorbed too readily which will result in dry skin. Emollients also have a special property called occlusion, which provides a layer of oil on the skin. This layer prevents the foot from drying up and can be very effective in treating dry skin disorders. If you can keep the skin on your feet healthy, this will substantially reduce the number of foot problems you will encounter in old age.
Proper footwear is another way to keep feet healthy. Shoes that fit well and provide proper support help prevent ingrown toenails and fallen arches.
Certain medical conditions such as diabetes or poor blood circulation increase the risk for foot issues. For individuals with any of these conditions it is extremely important to conduct regular foot inspections to make sure that there are no sores or infections present.
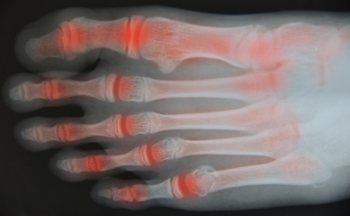
A PSA About PsA
Psoriatic arthritis, commonly abbreviated as PsA, is a form of arthritis that affects people who have a skin condition called psoriasis – although people without psoriasis can get it, too. PsA causes many of the joint symptoms associated with other types of arthritis, including pain, swelling, stiffness, and reduced mobility. More unique to PsA are symptoms such as toenail pitting, discoloration, and detachment, toe swelling, and itchy skin. If you have any type of arthritis affecting the lower limbs, a podiatrist can help you maintain or improve your foot and ankle health and mobility. To learn more about PsA and how to properly care for arthritic feet, please consult with a podiatrist.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Gregory T. Loo, DPM from Elite Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a term that is commonly used to describe joint pain. The condition itself can occur to anyone of any age, race, or gender, and there are over 100 types of it. Nevertheless, arthritis is more commonly found in women compared to men, and it is also more prevalent in those who are overweight. The causes of arthritis vary depending on which type of arthritis you have. Osteoarthritis for example, is often caused by injury, while rheumatoid arthritis is caused by a misdirected immune system.
Symptoms
- Swelling
- Pain
- Stiffness
- Decreased Range of Motion
Arthritic symptoms range in severity, and they may come and go. Some symptoms stay the same for several years but could potentially get worse with time. Severe cases of arthritis can prevent its sufferers from performing daily activities and make walking difficult.
Risk Factors
- Occupation – Occupations requiring repetitive knee movements have been linked to osteoarthritis
- Obesity – Excess weight can contribute to osteoarthritis development
- Infection – Microbial agents can infect the joints and trigger arthritis
- Joint Injuries – Damage to joints may lead to osteoarthritis
- Age – Risk increases with age
- Gender –Most types are more common in women
- Genetics – Arthritis can be hereditary
If you suspect your arthritis is affecting your feet, it is crucial that you see a podiatrist immediately. Your doctor will be able to address your specific case and help you decide which treatment method is best for you.
If you have any questions, please feel free to contact one of our offices located in Ahwatukee, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How to Care for Your Arthritic Foot
Arthritis is an inflammation of the joints and it can occur at any joint in the body, especially in the foot. It generally effects those who are older, however, it can occur at any age. Although there are many different forms of arthritis, there are three main types that occur in the foot. The three types are osteoarthritis, rheumatoid arthritis, and gout.
The primary cause of osteoarthritis is aging. As you age, cartilage degenerates around the joints which causes friction and pain. Obesity can cause osteoarthritis through mechanical stress. Injuries that damage joints can increase the probability as well. Finally, a family history of osteoarthritis can also increase chances of having it.
Rheumatoid arthritis occurs when the immune system attacks the joint linings and weakens them over a long time. While there is no known cause of rheumatoid arthritis, obesity and smoking can increase your chances of getting it. Women are also more likely to get it than men.
Gout is a form of arthritis that occurs when there is too much uric acid in your blood and painful crystals form in your joints. Men are more likely to have gout than women. People who are obese or drink alcohol often are also more likely to develop gout. Furthermore, having diabetes, heart disease, high blood pressure, high cholesterol, gastric bypass surgery or a family history of gout may increase your likelihood of developing the condition.
Symptoms of arthritis include pain, stiffness, swelling in the joints. These symptoms can make it harder and more painful to walk. Physical activity can increase pain and discomfort. Furthermore, joint pain can worsen throughout the day for osteoarthritis. Gout attacks generally last several days with the first few being the worst.
Diagnosis of gout includes either a joint fluid test or a blood test. X-ray imaging can detect osteoarthritis but not gout. On the other hand, there is no blood test for osteoarthritis. Rheumatoid arthritis is difficult to diagnosis. Doctors utilize family and personal medical history, a physical examination, and antibody blood tests to determine if you have rheumatoid arthritis.
Treatment varies for the different kinds of arthritis. Anti-inflammatory medication or steroids can help reduce pain from inflammation of the joints. Changing shoe types can help with some symptoms. Wider shoes can help with discomfort from gout and osteoarthritis. High heels should be avoided. Shoes with proper arch support and that take pressure off the ball of the foot can help with rheumatoid arthritis. Drinking lots of water can also help rid uric acid from the blood. Losing weight, improving your diet, and limiting alcohol and smoking can also help prevent or lessen the symptoms of arthritis.
If you are having trouble walking or pain in your feet, see a podiatrist to check if you have arthritis.
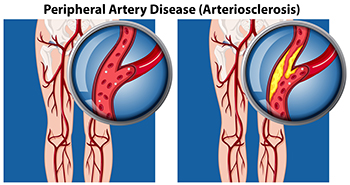
The Two Types of Peripheral Artery Disease
Peripheral artery disease (PAD) is a medical condition characterized by poor blood flow to the lower limbs. Though often asymptomatic in its early stages, PAD can eventually result in leg cramps and pain while walking, muscle weakness, coldness or numbness in the feet, and the formation of ulcers on the feet and lower legs. There are two types of PAD, occlusive and functional. Occlusive PAD occurs when something physically blocks or narrows the arteries. The most common cause of occlusive PAD is a buildup of a fatty substance, called plaque, along the artery walls. Functional PAD occurs when the blood vessels are not working properly. This is often caused by abnormal contractions, or muscle spasms, in the walls of the arteries. To learn more about PAD, please consult with a podiatrist.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with Gregory T. Loo, DPM from Elite Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
- Claudication (leg pain from walking)
- Numbness in legs
- Decrease in growth of leg hair and toenails
- Paleness of the skin
- Erectile dysfunction
- Sores and wounds on legs and feet that won’t heal
- Coldness in one leg
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact one of our offices located in Ahwatukee, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Peripheral Artery Disease
Peripheral artery disease (PAD), or peripheral arterial disease, is a circulatory problem in which there is a reduction of blood flow to the limbs due to narrowed arteries. When peripheral artery disease develops, the extremities do not receive enough blood flow; this may cause symptoms to develop such as claudication, or leg pain when walking. The legs are the most common site of peripheral artery disease.
Claudication, or leg pain when walking, is one of several symptoms that can develop due to peripheral artery disease. Other symptoms caused by the disease include painful cramping in the hips, thighs, or calves after certain activities; leg numbness or weakness; coldness in the lower leg or foot; sores on the lower extremities that do not heal; hair loss on the lower extremities; and a missing or weak pulse in the lower extremities. In more severe cases, pain may even occur when the body is at rest or when lying down.
Peripheral artery disease is typically caused by atherosclerosis, a condition in which fatty deposits build up in the arterial walls and reduce blood flow. Smoking, diabetes, obesity, high blood pressure, and high cholesterol are some of the risk factors for peripheral artery disease.
If you are experiencing pain, numbness, or other symptoms in the lower extremities, see your healthcare professional immediately. Diagnosed peripheral artery disease can be treated with various medications, angioplasty and surgery, exercise programs, or alternative medicine. It is important to consult a healthcare professional to determine the best treatment for you.
Who Needs an ABI Test?
 An Ankle-Brachial Index (ABI) test is a screening tool that is used to assess circulation in the lower limbs. During an ABI test, the doctor takes your blood pressure at various points along your arms and lower legs and compares the numbers to determine your risk of having full or partial blockages in the blood flow of your lower limbs. Not everyone needs an ABI test. They are typically done for people who are at risk of peripheral artery disease, a condition characterized by poor circulation in the extremities. People who are at risk of having peripheral artery disease include those with a history of smoking, high blood pressure, high cholesterol, diabetes, and atherosclerosis, as well as older adults and people who have a family history of peripheral artery disease. To learn more, please consult with a podiatrist.
An Ankle-Brachial Index (ABI) test is a screening tool that is used to assess circulation in the lower limbs. During an ABI test, the doctor takes your blood pressure at various points along your arms and lower legs and compares the numbers to determine your risk of having full or partial blockages in the blood flow of your lower limbs. Not everyone needs an ABI test. They are typically done for people who are at risk of peripheral artery disease, a condition characterized by poor circulation in the extremities. People who are at risk of having peripheral artery disease include those with a history of smoking, high blood pressure, high cholesterol, diabetes, and atherosclerosis, as well as older adults and people who have a family history of peripheral artery disease. To learn more, please consult with a podiatrist.
Vascular testing plays an important part in diagnosing disease like peripheral artery disease. If you have symptoms of peripheral artery disease, or diabetes, consult with Gregory T. Loo, DPM from Elite Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Vascular Testing?
Vascular testing checks for how well blood circulation is in the veins and arteries. This is most often done to determine and treat a patient for peripheral artery disease (PAD), stroke, and aneurysms. Podiatrists utilize vascular testing when a patient has symptoms of PAD or if they believe they might. If a patient has diabetes, a podiatrist may determine a vascular test to be prudent to check for poor blood circulation.
How Is it Conducted?
Most forms of vascular testing are non-invasive. Podiatrists will first conduct a visual inspection for any wounds, discoloration, and any abnormal signs prior to a vascular test.
The most common tests include:
- Ankle-Brachial Index (ABI) examination
- Doppler examination
- Pedal pulses
These tests are safe, painless, and easy to do. Once finished, the podiatrist can then provide a diagnosis and the best course for treatment.
If you have any questions, please feel free to contact one of our offices located in Ahwatukee, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Vascular Testing in Podiatry
In foot care, vascular testing may be required in the diagnosing and treatment of certain podiatric conditions. Vascular testing is particularly relevant for patients with high-risk diabetes, poor circulation, peripheral artery disease (PAD), and chronic venous insufficiency (CVI). Procedures typically involve the examination of blood vessels throughout the body for blockages or buildup.
Vascular testing is very important for the diagnosis of various conditions, including peripheral artery disease and chronic venous insufficiency, as these conditions can greatly affect one’s quality of life and cause pain in the lower limbs. Circulatory problems in the feet and ankles can reflect issues throughout the body, making testing of the blood vessels pertinent.
Testing methods vary between practitioners and can be specific to certain foot and ankle problems. Modern technology has brought about the ability to perform vascular testing using non-invasive methods, such as the cuff-based PADnet testing device. This device records the Ankle-Brachial Index (ABI)/Toe-Brachial Index (TBI) values and Pulse Volume Recording (PVR) waveforms. Contact your podiatrist to determine what vascular testing is available for your needs.
How Did I Get a Foot Wart?
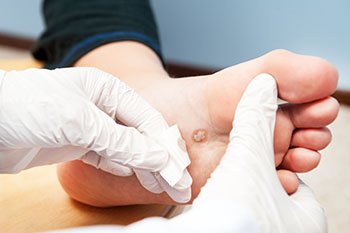 Plantar warts are rough growths that appear on the skin of the foot in response to a human papillomavirus (HPV) infection. This virus can enter the body through cuts or cracks in the skin. You can come in contact with HPV through direct skin-to-skin contact with an infected person, or through indirect contact with an infected surface, such as the towels, socks, shoes, or personal hygiene products of somebody who is carrying the virus. Warmth and moisture contribute to the virus’ growth, which is why people who wear closed shoes and socks and those who have sweaty feet are more likely to develop plantar warts. Plantar warts typically occur on parts of the foot that experience pressure and friction, such as the balls and heels of the feet. If you have a plantar wart, it is suggested that you see a podiatrist for treatment.
Plantar warts are rough growths that appear on the skin of the foot in response to a human papillomavirus (HPV) infection. This virus can enter the body through cuts or cracks in the skin. You can come in contact with HPV through direct skin-to-skin contact with an infected person, or through indirect contact with an infected surface, such as the towels, socks, shoes, or personal hygiene products of somebody who is carrying the virus. Warmth and moisture contribute to the virus’ growth, which is why people who wear closed shoes and socks and those who have sweaty feet are more likely to develop plantar warts. Plantar warts typically occur on parts of the foot that experience pressure and friction, such as the balls and heels of the feet. If you have a plantar wart, it is suggested that you see a podiatrist for treatment.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Gregory T. Loo, DPM from Elite Podiatry. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact one of our offices located in Ahwatukee, and Phoenix, AZ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.